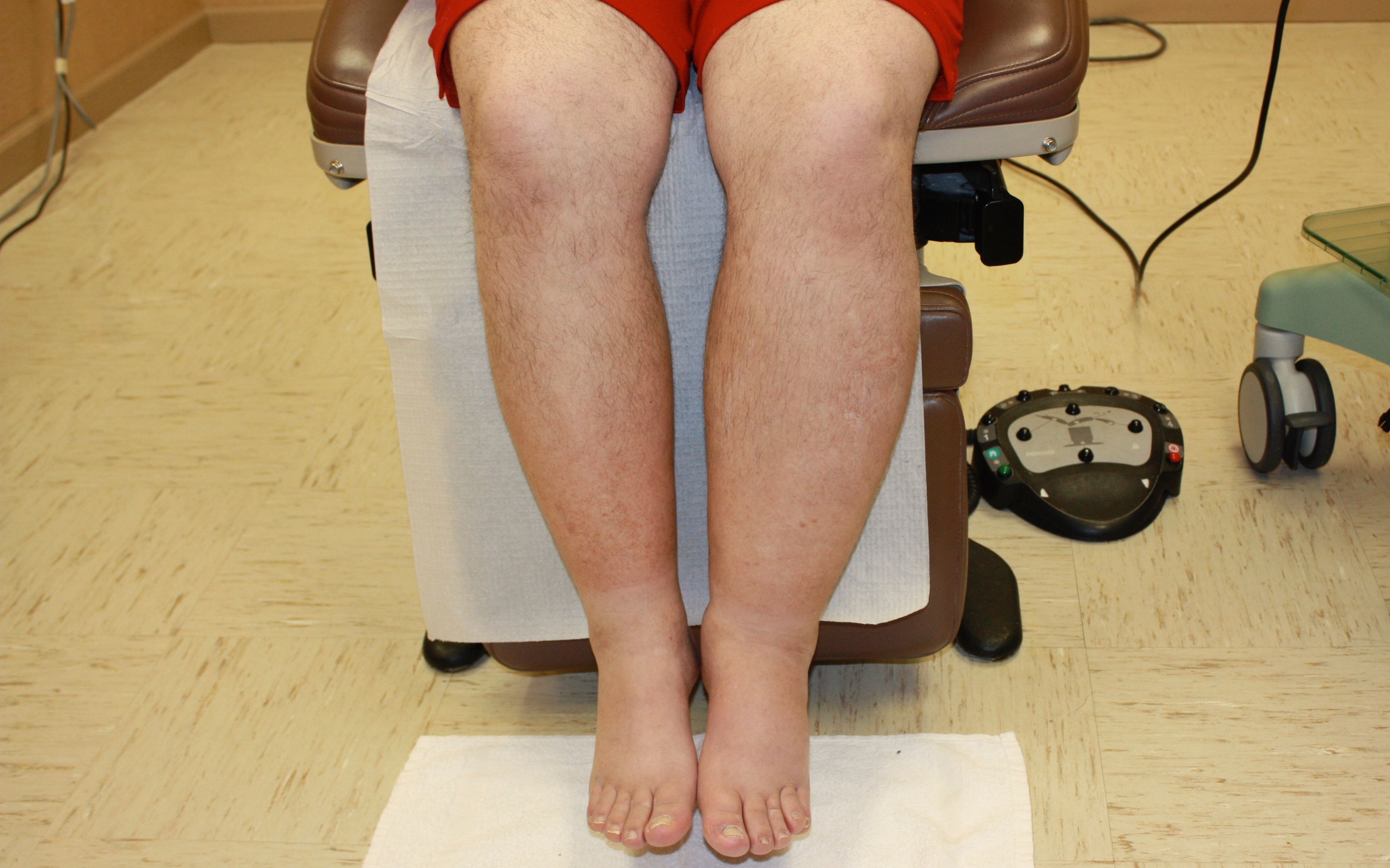
Lymphedema Treatment Fort Worth, TX
Lymphedema is swelling that occurs from the accumulation of fluid in the tissues. Normally, during the circulation of the blood, fluid from the bloodstream leaks into the surrounding tissue. In the tissues, the lymphatic system is an open ended microscopic system of thin walled vessels that collect the fluid and ultimately return the fluid to the bloodstream. Lymphedema occurs when there is an overproduction of the lymph fluid which overwhelms the lymphatic system, or impairment of the lymphatic vessels that remove the lymph fluid, the end result being an abnormal accumulation of fluid in the tissue. Lymphedema often results from venous hypertension, because the increased pressure in the thin-walled veins pushes more fluid out of the veins chronically. For this reason, lymphedema is often incorporated into the realm of vein medicine. However, a number of other disorders produce lymphedema unrelated to vein disease. These include genetic disorders, injury, infection, surgery, radiation therapy, and cancer. In tropical areas of third world countries, filariasis infection produced by a parasite is the most common cause of lymphedema. In the United States and developed countries, obesity is the most common cause of lymphedema.
Call Today to Schedule Your Appointment
Types of Lymphedema
Lymphedema is divided into two categories. Primary lymphedema is the result of developmental abnormalities of the lymphatic system and is felt in virtually all cases to be genetic or inherited. Secondary lymphedema is by definition caused by injury or another disease which alters either lymphatic production or elimination. Both have a number of causes.
Primary Lymphedema
A rare, inherited condition, primary lymphedema is caused by genetic abnormalities of lymph vessel development. These are seen more commonly in women, but can also occur in men. Primary lymphedema is divided into congenital lymphedema, lymphedema praecox, and lymphedema tarda. The features of each are as follows:
Congenital lymphedema
This form becomes apparent by the age of two years and represents only 10% of cases of primary lymphedema. All are felt to have a genetic origin. Some of the genetic disorders are well documented and specific gene mutation identified. Others are probably genetic based disorders, but lack a clearly identified gene mutation at this time.
Lymphedema Praecox
This represents 80% of all primary lymphedema. The age of onset is usually between the age of 2 and 25 years. It often appears during childhood or puberty. Most of the time it occurs spontaneously, but often the onset appears to be related to some minor injury or even an insect bite.
Lymphedema Tarda
Also called late-onset lymphedema because of the onset after age 35, lymphedema tarda often occurs much later in life. This form is also relatively rare, again comprising about 10% of primary lymphedemas. It is thought to have a hereditary or genetic cause because it often runs in families and is seen from one generation to the next.
Most experts also recognize that as more is known about lymphedema, many primary lymphedemas may ultimately prove to be secondary to other causes which have not been identified at this time.
Secondary Lymphedema
Secondary lymphedema arises from any condition or procedure that damages lymph nodes or lymph vessels, or conditions in which the amount of lymphatic fluid produced is increased, overwhelming the ability of the lymphatic vessels to remove the fluid. Causes of secondary lymphedema may include:
Surgery
If lymph nodes and lymph vessels are removed or cut during surgery, lymphedema may result. Lymph nodes are often removed in the underarm, groin or pelvic areas to treat breast cancer, gynecologic cancers, prostate cancer, testicular cancer, bladder cancer and melanomas, and lymphedema is often a side effect.
Radiation treatment
Radiation treatment can cause scarring and inflammation to lymph nodes or lymph vessels, which affects the flow of lymph fluid, causing lymphedema.
Cancer
Tumors from cancer that has metastasized may grow large enough to block lymph vessels, and restrict the flow of lymph fluid, resulting in lymphedema.
Infection
Lymph-node infections, either bacterial or fungal, can restrict the flow of lymph fluid. Infection may also be caused by parasites. Filariasis, which is caused by roundworms, is one such parasitic infection. Infection-related lymphedema is usually found in tropical and subtropical regions, and in developing countries.
Obesity
While most secondary lymphedema occurs due to damage to the lymphatic vessels, obesity appears to have a different mechanism. In obesity it is felt that the larger volume of tissue in the legs produces a larger area that requires removal of lymphatic fluid, and at some point the amount of fluid in the expanded tissue volume overwhelms the ability of the lymphatic vessels to remove the fluid. In other words, the soft tissue outgrows the lymphatic system. There may also be a component of lymphatic impairment due to chronic inflammation in the soft tissue and scarring of the delicate lymphatic vessels, but there is disagreement about the role of lymphatic impairment, and most experts feel the increase in the volume of tissue is the major cause of lymphedema related to obesity.
Symptoms of Lymphedema
Most lymphedema occurs in the arms or legs. Swelling may be barely noticeable or so extreme that using the arm or leg becomes impossible. In many cases, symptoms of lymphedema in the arm and leg include:
- Swelling, possibly including fingers or toes
- Aching or discomfort
- A full or heavy sensation
- Restricted range of movement
- Tight or shiny skin
- Lack of indentation in the skin when pressed
- Hardening and thickening of the skin
- Small warts or blisters that leak clear fluid
- Recurring infections
- Tighter-fitting rings and watches
Although most secondary lymphedema appears within three years of cancer surgery and treatment, it may also suddenly appear many years later.
Is lymphedema painful?
Lymphedema in advanced stages can be painful due to chronic swelling and the progressive inflammation and scarring that can occur with longstanding poorly controlled lymphedema. Reduction in the volume of fluid in the tissue of the affected arm or leg will reduce the degree of chronic inflammation and fibrosis (scarring) that occurs over time.
Treatment of Lymphedema
There is no cure for primary lymphedema. Secondary causes of lymphedema may improve over time if the underlying cause can be treated effectively, though often the damage done to the delicate lymphatic vessels is irreversible. Treatment for both primary and secondary lymphedema therefore focuses on reducing swelling and controlling pain, primarily through the use of compression in the form of garments, wraps, or pumps. It is notable that drugs are usually not effective to treat lymphedema, unless there is an infection. Diuretics (drugs that remove fluid from the body) also do not help, and may exacerbate symptoms. Lymphedema treatment often includes:
- Compression sleeves or stockings
- Exercise that incorporates gentle contraction of muscles in the affected limb
- Compression bandages that encourage lymph-fluid drainage to the center of the body
- Pneumatic-compression devices
- Massage therapy that helps to drain lymph fluid
Several of these treatments may also be combined depending upon the response to the therapy. Attempts to reduce the volume of the affected tissue surgically, and efforts to surgically reconstruct the lymphatic system are being pioneered, but have had limited success.
*The information about Lymphedema Treatment was reviewed by Board Certified Surgeon Dr. Michael Darnell. If you have any questions, please don’t hesitate to contact us using our contact form.