Chronic Venous Insufficiency Fort Worth, TX
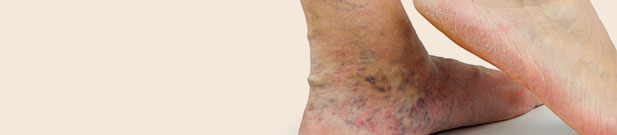
Chronic Venous Insufficiency
Your veins are like one-way streets with traffic meant to flow in only one direction. That can be more difficult in areas of the body where gravity can’t help the flow, such as the legs. Veins return blood to the heart from all of the body’s organs, and in the legs the blood needs to flow upward. With every step you take, the muscles in your feet and calves need to contract to squeeze the veins and help push the blood upward. To keep the blood from moving backward down the vein, veins have one-way valves.
Sometimes the venous wall and the valves stop working properly and blood collects, or pools, in the veins. This happens in a condition called chronic venous insufficiency (CVI). CVI can lead to varicose veins, swelling in the legs and ankles, itching skin on the legs and feet, and even skin infections. It is estimated that 40 percent of the people of the United States population have some degree of CVI.
Call Today to Schedule Your Appointment
What causes chronic venous insufficiency?
CVI occurs when the valves in the veins become damaged, allowing blood to leak backward. This can be a result of a blood clot in the deep veins of the legs, a disease known as deep vein thrombosis. It can also be a result of aging, extended sitting or standing, or obesity. CVI is more common in women and in people over the age of 50.
What are the risk factors for chronic venous insufficiency?
There are certain risk factors that make it more likely a person will develop CVI. These are the most important risk factors:
- Varicose veins
- Deep vein thrombosis
- Obesity
- Inactivity
- Extended periods of sitting or standing
- Being a female
- Being over the age of 50
- Pregnancy
- Smoking
How do I know if I have CHRONIC VENOUS INSUFFICIENCY?
A person shouldn’t just live with CVI. The seriousness of the disease increases as it progresses. If you show any of these symptoms, you need to see the team at the Reeder Vein Institute because the problem will not go away on its own.
Symptoms of CHRONIC VENOUS INSUFFICIENCY include:
- New varicose veins
- Tired, aching legs
- Swelling in the lower legs and ankles, particularly after periods of standing
- Leathery-looking leg skin
- Itching skin on the feet and legs
- Cramping
- Changes in skin color
- Skin sores (ulcers)
Sores, known as stasis ulcers, develop when pressure and swelling in the lower legs increases to the point where the tiniest blood vessels burst. This gives the surface skin a reddish-brown color. This tissue inflammation can lead to ulcers on the surface that can be difficult to heal and can become infected.
CVI is often also associated with varicose veins, those twisted, enlarged veins just under the surface of the skin.
How do you treat CHRONIC VENOUS INSUFFICIENCY?
Once the team at Reeder does a complete evaluation, including a detailed ultrasound examination, we’ll settle on a treatment plan for your chronic venous insufficiency. As with most diseases, early treatment delivers the most successful treatment. Treatment usually consists of a combination of compression therapy, endovenous ablation, and ultrasound-guided sclerotherapy.
casual treatment approaches we often use first for CHRONIC VENOUS INSUFFICIENCY:
- Regular exercise, particularly walking
- Weight loss if the patient is obese
- Avoiding long periods of sitting or standing (if you do need to do this, take periodic breaks to flex and extend your legs and to elevate your feet)
- Leg elevation when sitting or lying down (legs above your heart)
- Compression stockings
- Antibiotics to correct any skin infections
Sclerotherapy is a long-used method of addressing spider veins and small varicose veins. We inject a salt solution into the vein. This irritates the lining of the blood vessel, causing it to swell and stick together, closing off the vein.
Endovenous thermal ablation delivers similar results to sclerotherapy, but uses different means to get there. In this technique, laser or high-frequency radio waves are sent directly into the varicose vein where the energy converts to heat. This heat damages the vein wall, closing the vessel off. In both sclerotherapy and endovenous thermal ablation, blood in the vessel is re-routed by the body to an adjacent, hopefully healthier, vein.
Far more rarely, we may recommend surgery to correct your CVI. This can include ligation and vein stripping, ambulatory phlebectomy, or a vein bypass.
*The information about Chronic Venous Insufficiency was reviewed by Board Certified Surgeon Dr. Michael Darnell. If you have any questions, please don’t hesitate to contact us using our contact form.
